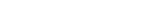Diabetic Ulcers
The clinical evidence from individual studies on LLLT for wound healing in the challenging situation where diabetic ulcers have developed is supportive of benefit from the treatment across in-vitro and non-clinical data, and by the pooled evidence of meta-analyses. The clinical studies demonstrate a moderate beneficial effect on diabetic ulcers over both the short and longer term.
Consistent with our customer feedback, LLLT was also reported in studies to be a pain-free, cost-effective treatment without adverse effects and indeed very few reports of complications were found in the relevant studies. In relation to the state-of-the-art alternatives, it offers a non-invasive method of treatment with a risk to the patient that is very significantly lower than that of any alternative therapy.
Despite considerable variation in treatment regimens and calls for more well-designed trials to be undertaken, all 22 studies on LLLT for diabetic ulcer treatment systematically identified for review reported improved wound healing in terms of either a reduction in ulcer area (cm2) from baseline or between treatment groups, the percentage reduction in ulcer size, or in the proportion (%) of patients with completely or partially healed ulcers.
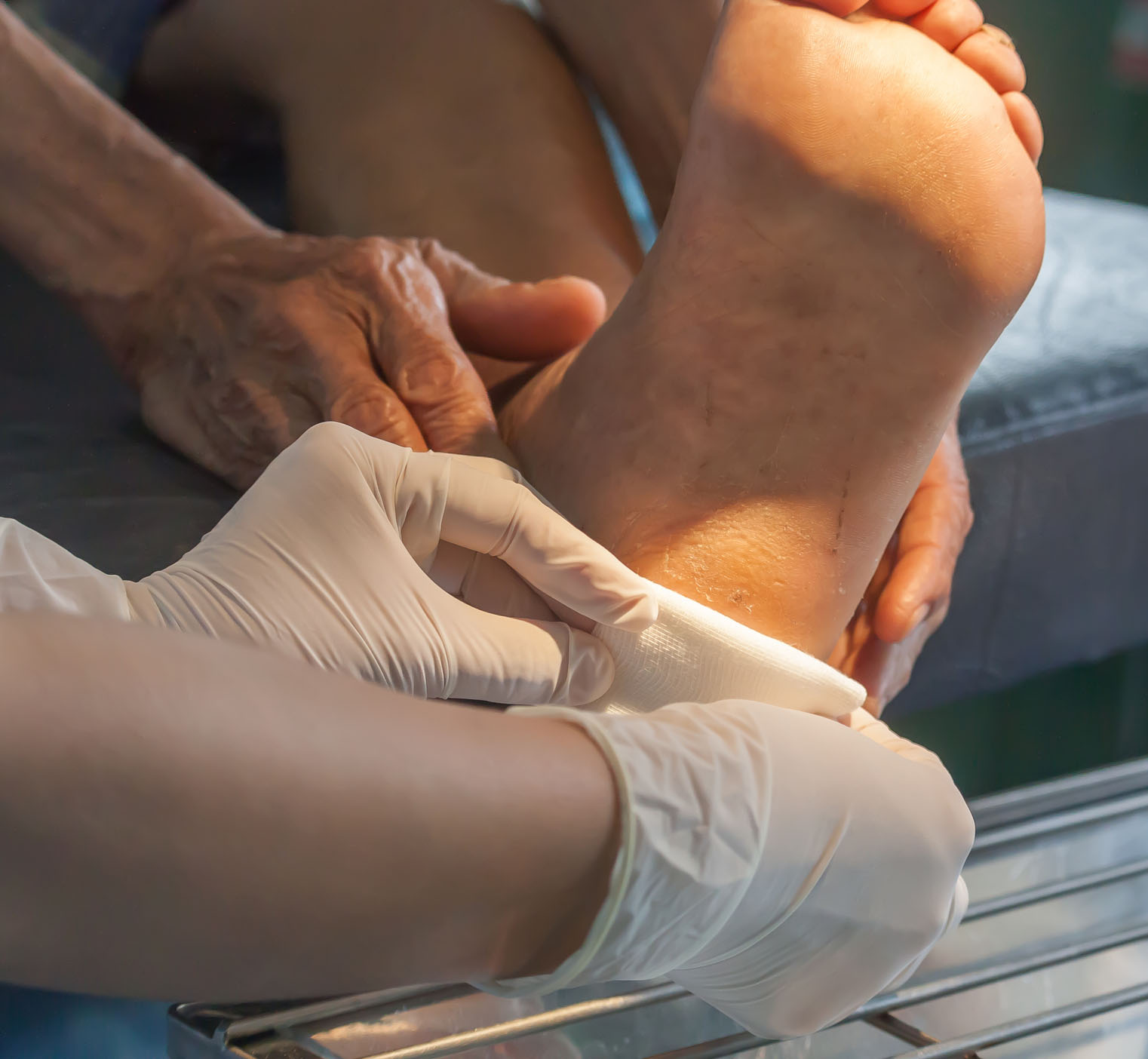
Wound Healing Action
Wound healing was one of the first applications of LLLT: the therapy can affect all three phases of wound healing: the inflammatory phase, in which immune cells migrate to the wound, the proliferative phase, which results in increased production of fibroblasts and macrophages, and the remodelling phase, in which collagen deposition occurs at the wound site and the extra-cellular matrix is rebuilt.
LLLT is understood to promote wound healing by inducing the local release of cytokines, chemokines, and other biological response modifiers that reduce the time required for wound closure, and increase the mean breaking strength of the wound. This result is achieved by increasing the production and activity of fibroblasts and macrophages, improving the mobility of leukocytes, promoting collagen formation, and inducing neovascularisation (Chung et al. 2012, Hamblin 2017).
In-vitro studies using Omega Laser equipment demonstrate how light irradiation affects macrophage function to either stimulate or inhibit fibroblast proliferation. The in-vitro studies also illustrate that the results obtained are dependent upon the light wavelength, pulse frequency and energy density used, and consequently the importance of determining appropriate irradiation conditions.
Non-clinical studies have shown that light irradiation can stimulate mast cell degranulation which may influence tissue repair and also how LLLT can ameliorate the effect of dermal necrosis following X-irradiation.
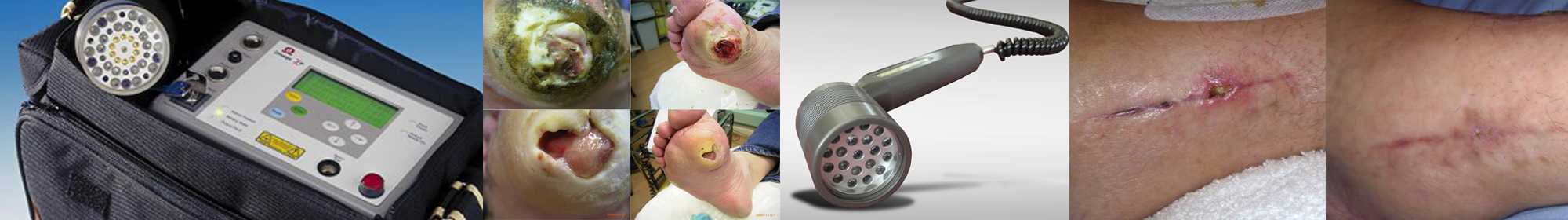
“After having months of treatment for various leg ulcers from my doctors and nurses, they were not responding. I was referred to Ashdown Clinic, where I received laser treatment. This was successful, and the ulcers were completely healed.”
Case Study
History
Female patient in nursing / residential home with 23 years leg ulceration. Previously treated using Florozene and Alginate dressings.
Treatment
Dose: 8 J/cm2 per treatment (2 minutes per point)
Wavelength(s): Multiple wavelengths
Pulsing: mixed low, medium and high frequencies
Probe: 46 Diode Cluster Probe
Frequency/intervals: Once every 2 weeks
Outcome
Patient reported being pain-free relatively early on in treatment but complete healing of chronic leg ulceration took a total of 9 months (including a 4 month break due to unrelated illness). Quickly able to socialise, no pain and completely healed.
Contact us
Contact Omega to discuss the application of laser in your practice.
Call +44 (0) 1787 477551 or email info@omegalaser.co.uk